If you’ve ever had a bout with red, itchy welts on your skin, you likely had a case of the hives. But did you know that hives could be associated with a problem with your thyroid?
Several studies have linked hives and thyroid disease (particularly Hashimoto’s disease). But why does this occur, and is there anything you can do about it? As we wrap up Thyroid Awareness Month, let’s dive into why these two conditions are connected – and what you can do if you’ve been dealing with chronic hives.
What are hives?
Hives (or their more technical name, urticaria) are a common skin rash that can be triggered by a range of things – including allergic reactions to food, medications, or insect bites, as well as infections, sun or cold exposure, anxiety, or stress.
Hives can occur as a single incident, or they can happen over and over for several weeks at a time without an obvious trigger. If your hives stick around for more than six weeks, your hives may be considered chronic.
How are hives and thyroid disease connected?
While we mentioned a few potential causes of hives, there’s one association we should also mention – and that’s thyroid disease. One 2018 article noted that, in patients with chronic hives, anywhere between 25 to 30 percent of patients were found to have thyroid antibodies, and Hashimoto’s disease was later diagnosed. [1] In another 2020 review, hives were associated with autoimmune thyroid disease (or autoimmune thyroiditis) in anywhere between 4.3 to 57.4 percent of patients with chronic hives. [2]
Scientists are still working out why hives and thyroid disease are associated. One 2013 study theorized that the hives could be connected to autoimmunity (when the immune system attacks the body) due to hives occurring with other autoimmune disorders such as type 1 diabetes, rheumatoid arthritis, and celiac disease. [3]
While we don’t know exactly why hives occur in people with Hashimoto’s disease, it’s important to note that hives could be an early sign that your thyroid isn’t functioning properly. Because standard thyroid testing only examines TSH levels, it’s important to also test for thyroid antibodies such as TPO.
What treatment exists for hives caused by Hashimoto’s disease?
The 2020 review found studies which suggested that treatment with antithyroid drugs or levothyroxine (a thyroid hormone) could help reduce the recurrence of hives. [2]
In the 2018 study, which examined 72 patients with chronic hives and thyroid antibodies, patients who took both levothyroxine and an antihistamine (a drug that treats allergic reactions) recovered faster than people who only took the antihistamine. [1] Another 2011 study of patients with chronic hives suggested that thyroid screening may be useful for all patients who are experiencing chronic hives. [4]
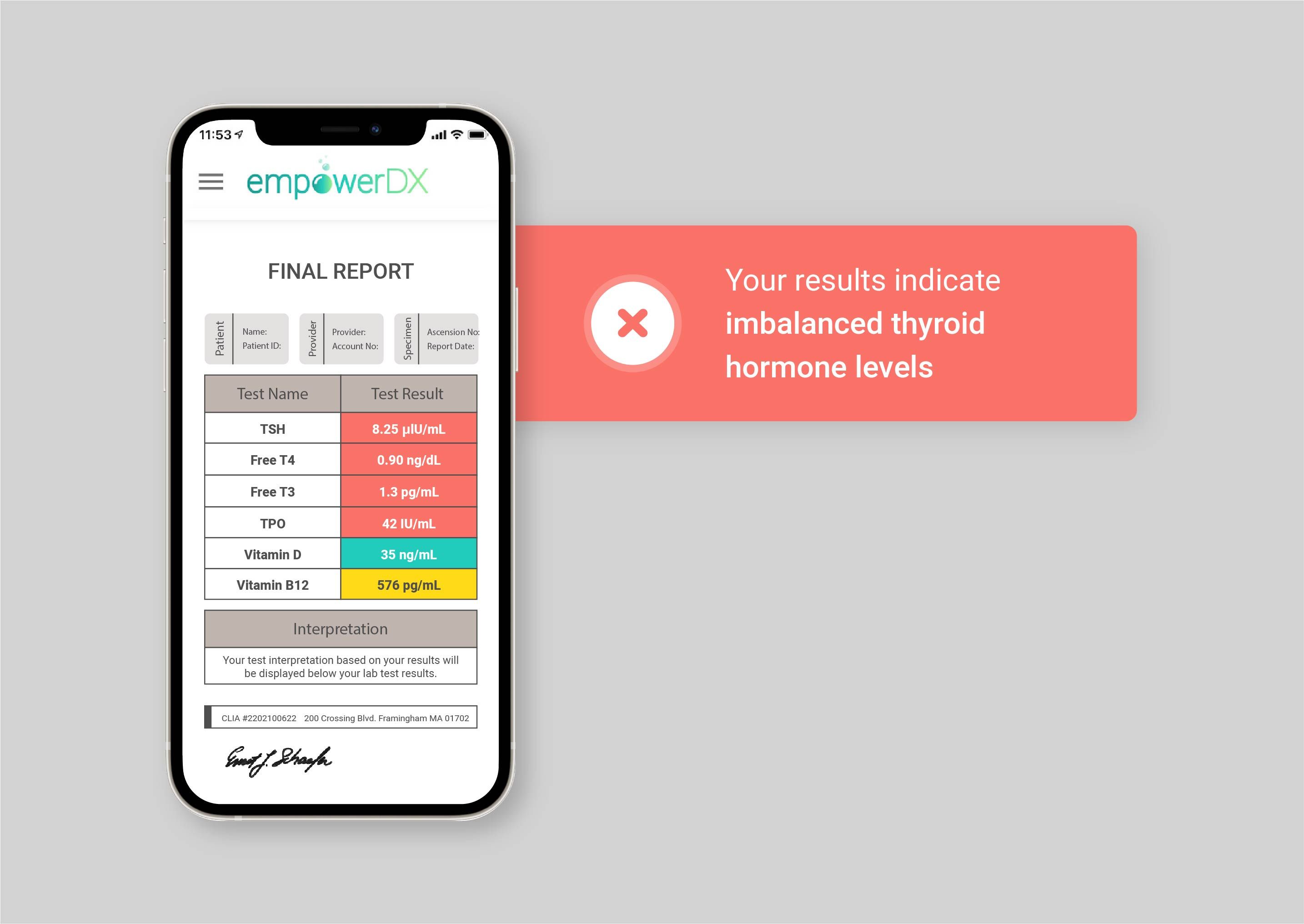
So what does all this research mean for you? For starters, it’s important to talk to your doctor or healthcare provider if you’ve been experiencing frequent bouts of hives – especially if they’ve lasted longer than six weeks and could be considered chronic.
Standard thyroid testing typically only examines your TSH levels, so it may miss the thyroid disease that could be connected to your hives. Be sure you’re testing beyond TSH levels, and make sure you test for TPO levels – like with an at-home thyroid test from empowerDX.
Dealing with unexplained conditions like hives can be frustrating – but there are options available to you to help you get answers and move forward.
Sources
[1] Najafipour, Farzad, et al. “Relationship between Chronic Urticaria and Autoimmune Thyroid Disease.” Journal of Advanced Pharmaceutical Technology & Research, vol. 9, no. 4, Oct. 2018, p. 158., doi:10.4103/japtr.japtr_342_18.
[2] Gonzalez-Diaz, Sandra Nora, et al. “Chronic Urticaria and Thyroid Pathology.” World Allergy Organization Journal, vol. 13, no. 3, Mar. 2020, p. 100101., doi:10.1016/j.waojou.2020.100101.
[3] Fraser, Kathleen, and Lynne Robertson. “Chronic Urticaria and Autoimmunity.” Skin Therapy Letter, vol. 18, no. 7, 1 Dec. 2013.
[4] Nuzzo, Vicenzo, et al. “Idiopathic Chronic Urticaria and Thyroid Autoimmunity.” Dermato-Endocrinology, vol. 3, no. 4, 2011, pp. 255–258., doi:10.4161/derm.3.4.17066.


